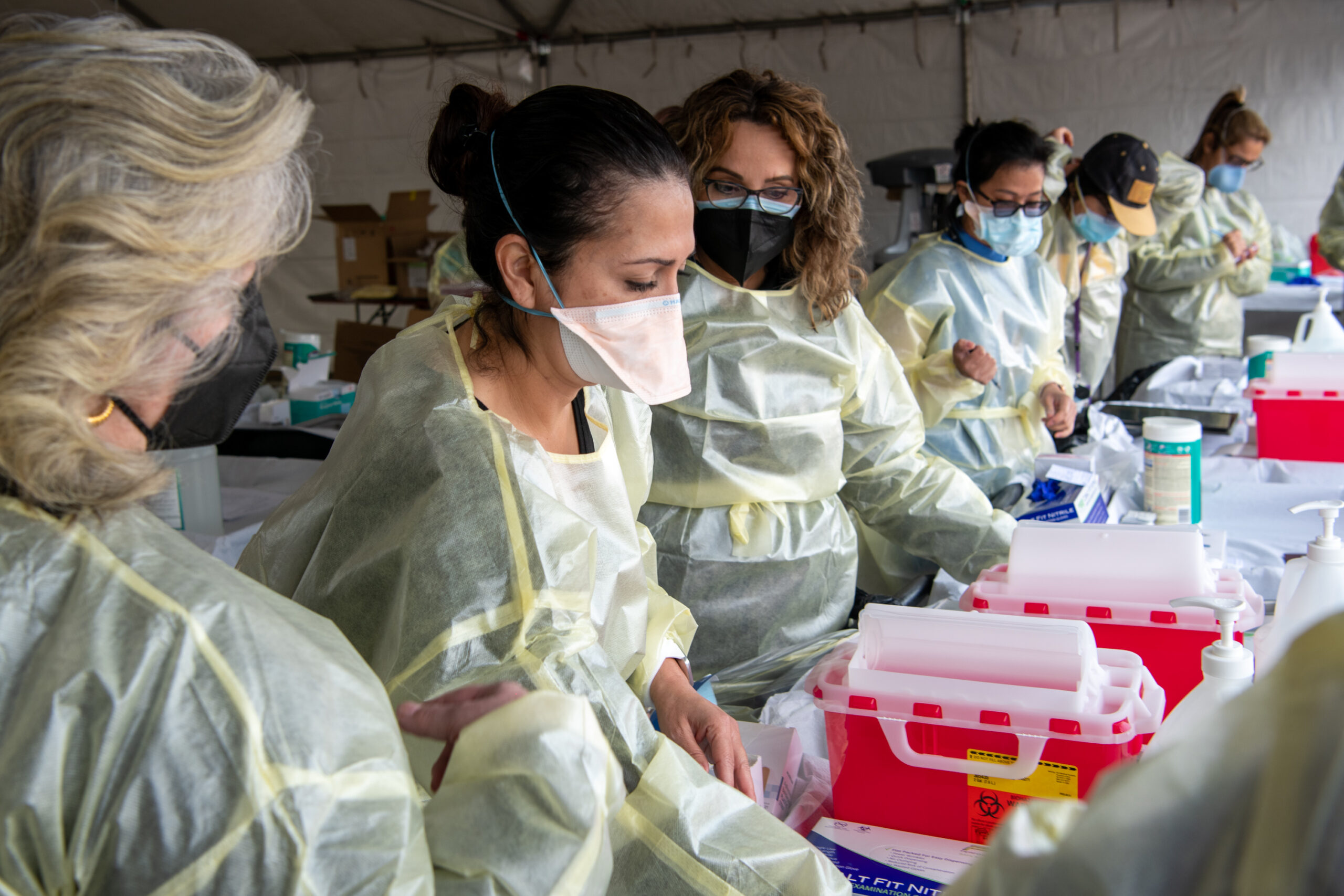
Despite the high number of deaths in older adults from the Omicron surge, a significant number remain “un-boosted” — only 29.5% of people 65 and older are “fully boosted” with both first and second booster shots.
A briefing hosted by Ethnic Media speakers discussed the challenges of getting older adults fully boosted, the efficacy of boosters against new variants for older adults, where access issues persist for isolated populations, and the need for sustained public education campaigns to combat complacency and disinformation.
Susan DeMarois, Director, California Department of Aging shared that the population of older adults has been hardest hit. 70% of covid deaths in California are our older adults. She also shared that she had friends who had tested positive for covid and this is very common in the older populations especially older adults of color.
Dr. Sara Tartof, Infectious Disease Epidemiologist, Kaiser Permanente Southern California explained how the efficacy of vaccines dwindles over time, especially for immunocompromised older adults. Sharing the work done to gain insights into the vaccines and waning from covid vaccines and boosters. They are also looking at the variants and how well the vaccines work. She quoted a study written in the New York Times paper that gave insight into the trends. The results showed that 3doses gave more protection and the takeaway was that there is a significant waning of protection in the first two doses. The third dose gives a big boost. In immunocompromised adults, it is absolutely important that this population gets boosted up with the third dose. Now we are into four doses in which there is still a drop-off. The recommendation is five doses.
Denny Chan, Directing Attorney, Justice in Aging talked about the importance of keeping the pressure on as covid has affected us all. As an advocate, he has been involved in making sure there is equitability in distributing covid vaccines. Older adults tend to experience higher hospitalizations and death rates. We must call attention to covid and older adults. Black, Hispanic, American Indian, and older, etc. are most vulnerable. Higher rates in communities of color. Higher rates of infection and spread where there are people of color and older adults in housing or nursing facilities. Worth noting that the Latino population in California is 20% but makes up almost 85% of deaths. The numbers are going up 13% in the test positivity rate. However, there is an undercount as not everyone is getting tested. On a positive note, there are now ways to get access to get tested or get vaccinated which did not exist at beginning of the pandemic. Vaccines are getting approved much more for different groups. Unvaccinated groups are more likely to get covid, be hospitalized, or dead from covid. The data shows that there is a need to have multiple strategies for getting people vaccinated particularly in older adults and older adults of color.
Roberto Velasquez, President & CEO, Southern Caregiver Resource Center, serving San Diego and Imperial Counties – Working with vulnerable older adult caregivers taking care of older adults talked about the data on where San Diego stands right now on covid. The staggering numbers showed how important it is to take covid seriously. Go to www.caregiver.org to find resources if you are a family caregiver. Caregivers are 48% between 45-64 and so are adult children taking care of parents. 51% of adult children and 31% are spouses. Family caregivers who take care of parents at home receive no paid help and report mental anguish. In addition to covid, it exacerbates the situation. He also shared the resources his office has done to alleviate families who are caregiving. Caregivers need support and with help can navigate the challenges of caregiving.